Surfactant and COVID-19
The FLARE Four
- Pulmonary surfactant is a complex mixture of lipids and proteins synthesized in alveolar epithelial cells that is essential to stability of the airspaces and simultaneously contributes to innate immune function. Alveoli are, in some superficial ways, similar to “tiny bubbles” - their stability depends on a balance between surface tension and transpulmonary “pressure”. Alveolar instability and disruption of surfactant activity is a hallmark of lung diseases like ARDS
- Some forms of acute lung injury, particularly in neonates, are effectively treated with surfactant administration and provide proof of concept for surfactant-based therapy of ARDS
- To date, clinical trials have failed to identify a clear signal for mortality benefit of surfactant replacement in unselected ARDS patients
- The biologic plausibility of surfactant therapy for ARDS is strong. Prior trials do demonstrate safety and have identified a suggestion of benefit in forms of ARDS driven by primary direct lung injury. COVID-19 associated respiratory failure (a primary lung process) provides a unique and valuable opportunity to revisit the utility of surfactant therapy in a large ARDS cohort with a single etiology
Many people are saying...we should try surfactant for COVID-19 ARDS
Subscribe to the latest updates from FLARE Advances in Motion
"Let’s Get (Bio) Physical”: The Biophysics of Surfactant
What are surfactants?
Liquids exhibit varying degrees of surface tension depending on their relative degrees of cohesion (attraction of molecules to themselves) versus adhesion (attraction to other types of molecules). A highly cohesive liquid such as water will adopt a configuration which maximizes water-water intermolecular interactions. This explains the formation aqueous droplets in oils – hydrophilic vinegar and water much prefer to interact with themselves than with the hydrophobic olive oil in your vinaigrette. We are all familiar with this property by way of detergents – the ability to solubilize grease in water is useful for washing dishes or “cars”.
At the interface between air and a cohesive liquid like water, the water molecules on the surface have fewer molecular interactions with other water molecules than the molecules not at the surface (which are surrounded entirely by other water molecules). Molecules on the surface will therefore be in a less energetically favorable state - this means that creating the interface requires energy. The cost of forming the interface may be expressed as an energy per unit area or a force per unit length. A force per unit length is a tension. Surface tension is, in part, responsible for the shape of “raindrops” (Granger 1995).
Surfactants (SURFace ACTive agents) are molecules which have both hydrophilic (“head”) and hydrophobic (“tail”) regions. Accumulation of surfactants at the air-liquid interface therefore decreases the energetic cost of forming the interface; in other words, they reduce surface tension.
As an interface between epithelial tissue (hydrated) and the external environment (air), the lung is subject to many of the same physical constraints as salad dressing or dish soap. In particular, because surface tension tends to reduce the radius of an air-liquid interface, alveoli and terminal airways have a natural tendency to collapse. Surface tension, in fact, supplies a major portion of the elastic recoil force of the lung. Re-opening collapsed regions of lung (such as may occur in ARDS) requires overcoming not only elastic recoil, but also the substantial liquid-liquid cohesion that tends to keep small airways and alveoli “stuck” closed. This phenomenon was demonstrated experimentally nearly 100 years ago by van Neergaard (v. Neergaard 1929), who inflated de-gassed pig lungs either with saline or with air and concluded that “surface tension is responsible for the greater part of total lung recoil compared to tissue elasticity”. It soon became clear that the lung employs some method to mitigate these surface tension effects and, by the 1950s, “pulmonary surfactant” had been identified and characterized.
The surface tension lowering properties of surfactant are dynamic, meaning surfactant activity changes with lung volume. On deflation, surfactant reduces lung surface tension to near zero! The full biophysical basis for these effects is complex and beyond the scope of this FLARE, so we direct interested readers to an excellent review by Pérez-Gil (Pérez-Gil 2008). In short, surfactant activity lowers alveolar opening pressure (i.e. increases compliance) and stabilizes against alveolar collapse. The consequences of surfactant activity on the pressure-volume curve of the lung are depicted in Figure 1 and highlight its central role in maintaining normal pulmonary mechanics.
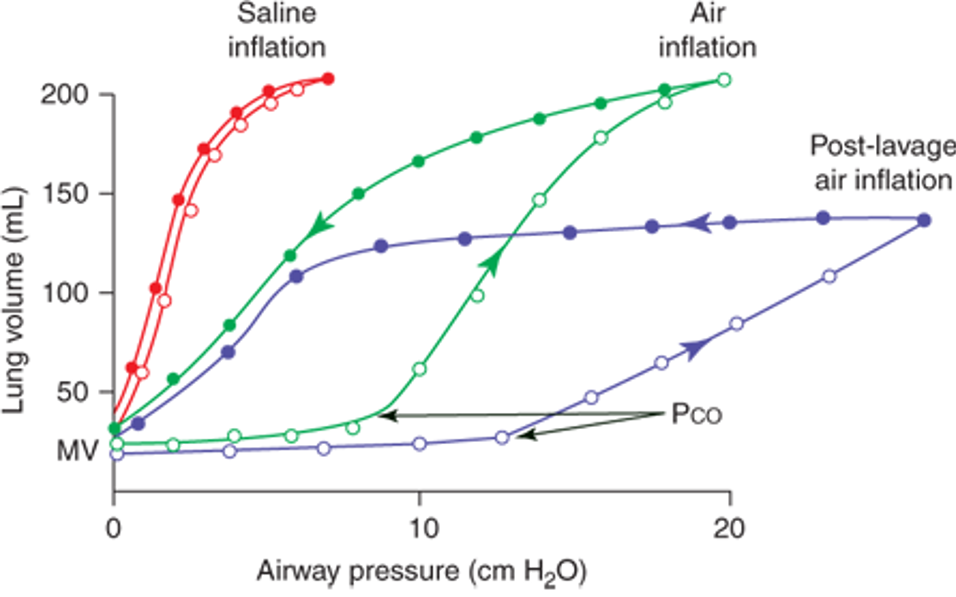
Figure 1
Pressure-volume curves from normal (green), saline-inflated (red), or surfactant-stripped (blue) lung illustrating surface tension-dependent changes in compliance and hysteresis. Surfactant-stripped lung requires higher opening pressure and has lowest compliance. MV = minimal volume (the volume to which the lung naturally collapses), Pco = critical opening pressure (the pressure required to recruit previously atelectatic units) [from Lechner, Matuschak, and Brink “Respiratory: An Integrated Approach to Disease”].
Biology of Surfactant
Decades of investigation have yielded a detailed understanding of mammalian surfactant synthesis and biophysical properties. Surfactant is a complex mixture of proteins and lipids synthesized by alveolar type II pneumocytes and packaged in specialized lysosome-related organelles (lamellar bodies) before regulated secretion. Surfactant is composed primarily (~80% by mass) of phospholipids such as dipalmitoyl-phosphatidylcholine (DPPC) which look and act much like detergents, having a hydrophilic phospho-head group and a hydrophobic acyl tail. Surfactant proteins (~5% of surfactant by mass) promote the rapid spreading of surfactant across the enlarging air-liquid interface during inflation (e.g. surfactant proteins B and C) and participate in innate immunity (e.g. surfactant proteins A and D) (McCormack and Whitsett 2002). Upon secretion, surfactant rapidly adopts a complex multi-layered organization in the alveolus, with an air-liquid interface film as well as a “sub-phase” from which additional surfactant molecules can mobilize as alveoli change size and shape during breathing (Figure 2). Surfactant is continually recycled, a process which involves both type II pneumocytes and alveolar macrophages.
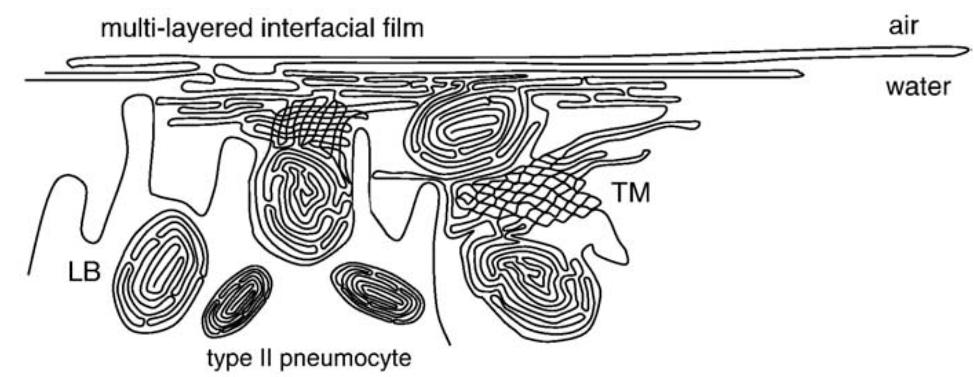
Figure 2
Surfactant is secreted by type II pneumocytes into a complex film at the alveolar surface. LB, lamellar body; TM, tubular myelin (a form of surfactant sub-phase) (Pérez-Gil 2008).
The specialized chemical and biophysical properties of surfactant are ultimately responsible for its mechanical effects on the lung.
Lessons From Pediatric Respiratory Failure
What happens when surfactant is absent or dysfunctional?
From what we have reviewed thus far, one might predict that loss of surfactant activity would be poorly tolerated. In an elegant 1959 manuscript, Mary Ellen Avery (working in Boston with Jere Mead) showed that lung homogenates from infants who died of hyaline membrane disease had less ability to lower surface tension than those from individuals who died of other causes - suggestive of the absence of a “surface active material” in the neonates. The pathophysiological mechanism they proposed still forms the basis for what we now know as neonatal respiratory distress syndrome (RDS). In brief, lack of surfactant results in an increased opening pressure for affected lung units, predisposing to collapse of airspaces in the first hours of life and the need to generate more negative pleural pressures to maintain airway patency. The larger negative pleural pressures contribute to edema and inflammation ensues, resulting in further surfactant inactivation and progressive hypoxemic respiratory failure. The central role of surfactant per se in driving RDS is further reinforced by genetic mutations which inactivate or alter surfactant protein B (SPB), the chief protein involved in efficient surfactant spreading and monolayer formation. Genetic SPB deficiency results in lethal neonatal lung injury with a clinical pattern similar to RDS, and polymorphisms in and around the SFTPB gene are associated with increased risk of RDS (Floros et al. 2006; Marttila et al. 2003).
Is there a role for exogenous surfactant in treating lung disease?
The appreciation that surfactant deficiency underlies RDS naturally led to intense efforts to replace or augment surfactant activity in critically ill children. In the 1980s, dozens of trials examined a large variety of surfactant preparations for the treatment of RDS. The wealth of accumulated evidence has led to strong recommendations for the administration of surfactant to decrease mortality in neonatal RDS (Polin et al. 2014).
Notably, exogenous surfactant has also proven beneficial in some pediatric settings even when the inciting insult is not primary surfactant deficiency. The best established setting is meconium aspiration syndrome (MAS), which leads to a form of hypoxemic respiratory failure characterized by increased surface tension and decreased lung compliance (Chen, Toung, and Rogers 1985) – potentially driven by stripping of surfactant from gas exchange surfaces (Clark et al. 1987). Remarkably, surfactant administration to neonates with MAS improves oxygenation indices and reduces the need for extracorporeal membrane oxygenation (ECMO) (El Shahed et al. 2014). Administration of surfactant to neonates with hypoxemic respiratory failure requiring ECMO (from any cause) also reduced lengths of ECMO need (Lotze et al. 1993). Together, these observations suggest that, at least in newborns, there may be generalizable benefits associated with surfactant administration in forms of hypoxemic respiratory failure characterized either by primary or secondary surfactant dysfunction.
Is There a Role for Surfactant Administration in ARDS or COVID-19?
Is surfactant really dysfunctional or deficient in ARDS?
ARDS, initially an acronym for “adult” respiratory distress syndrome, was so-named partly for its similarity to neonatal RDS – particularly the clinical findings of reduced lung compliance and histological evidence of hyaline membranes. Indeed, in the first report of what would come to be known as ARDS, Ashbaugh and colleagues write of pulmonary surfactant (yet to be characterized biochemically): “the theoretical basis for its presence is convincing, and indirect measurements seem to indicate that its loss is associated with the development of the clinical, physiological, and pathological conditions seen in the 12 patients in this series” (Ashbaugh et al. 1967). As a rather humbling aside, these authors a half century ago identified PEEP as a valuable therapy for this new disease and concluded that corticosteroids, antibiotics, alpha-adrenergic blockade, inotropes, and high-tidal volume intermittent mandatory ventilation were all of “doubtful value”.
Given the histological similarities between acute respiratory distress syndrome (ARDS) in adults and pediatric RDS, abnormalities in surfactant quantity and/or function have been proposed for years to drive or exacerbate ARDS. Subsequent work has revealed reductions in surfactant phospholipid concentrations and composition, as well as increased surface tension in ARDS patient samples (Dushianthan et al. 2012) consistent with this hypothesis.
In a “sign of the times”, surfactant therapy is among the previously studied therapies in ARDS which have been proposed for use in COVID-19. Like ARDS from other causes, SARS-CoV-2 infection also has features that resemble neonatal RDS such as hyaline membrane formation on pathologic samples (Xu et al. 2020). Type II pneumocytes are at least one of the alveolar cell types infected by SARS-CoV-2 (Rockx et al. 2020), and are the cells responsible for production of surfactant. Biopsy samples from COVID-19 as well as SARS patients have identified evidence of viral inclusions in these surfactant-producing cells (Zhang et al. 2020). Furthermore, if so infected, it is plausible that lysosomal trafficking and secretion (as is required for surfactant) might be impaired given the endolysosomal pathway by which beta-coronaviruses enter host cells.
Why hasn’t surfactant administration been effective in treating ARDS?
Surfactant administration has been studied in several adult ARDS trials but has thus far failed to improve mortality or to increase ventilator-free days. After early, small pre-clinical studies showed some promise, a large RCT (Anzueto et al. 1996) studied the use of aerosolized surfactant in sepsis-induced ARDS. In addition to the use of aerosolized delivery (which may have resulted in inadequate alveolar delivery) this study used a phospholipid-only surfactant preparation (i.e. no surfactant proteins). Two later large RCTs therefore tested liquid, recombinant surfactant protein C-incorporating lipid formulations which were instilled directly into the airway via catheter (Spragg et al. 2004). These trials, however, were negative as well.
There are a number of challenges in interpreting these results. First, these studies largely occurred in the pre-ARDSnet era - meaning they did not consistently employ low tidal volumes. It is possible that a benefit of surfactant was obscured by the harm associated with now outdated ventilatory practices. This difficulty arises in interpreting any older study in ARDS, but is, perhaps, particularly pertinent to surfactant trials since ongoing atelectrauma may have directly antagonized the effect of the therapy. Another difficulty is the heterogeneous nature of surfactant products and delivery methods used in various trials. It may be that surfactant failed to show benefit despite strong biologic plausibility simply because the administered surfactant failed to reach its intended target in the adult lung. Filoche and colleagues recently pointed out that intratracheal administration of surfactant is fundamentally different from administration of other drugs in which it may be reasonably assumed that drug quickly and homogeneously distributes throughout the relevant compartment (the intravascular compartment, for example, in the case of intravenous drugs). A bolus of surfactant in the trachea will be driven to the alveoli by inspiratory flow but will leave a thin film on the airway surfaces as it travels, thus decreasing its volume. In addition, the liquid drug is not likely to distribute evenly into both daughter branches at an airway bifurcation if one branch corresponds to a more gravitational-dependent route. Furthermore, Filoche and colleagues used modeling methods to show that the neonatal and adult lungs differ structurally in ways that would predict inefficient and imbalanced delivery of surfactant in adults if given using standard methods (Filoche, Tai, and Grotberg 2015).
On the other hand, data from Lu and colleagues suggest that surfactant administration can, indeed, augment lung aeration in ARDS (Lu et al. 2010) and there is in fact high-quality evidence to suggest oxygenation indices are improved as well (Spragg et al. 2004; H. Meng et al. 2012). Importantly, these studies generally used early and limited duration surfactant administration and leave open the possibility that sustained treatment might provide additional benefit. Alternatively, as appears true from studies of inhaled pulmonary vasodilators, it may be the case that improved oxygenation does not necessarily improve outcomes in ARDS. Nevertheless, in the end, multiple trials have failed to show a benefit. These data have been summarized in multiple recent meta-analyses and systematic reviews (S.-S. Meng et al. 2019; Lewis et al. 2019) and in Figure 3 below.
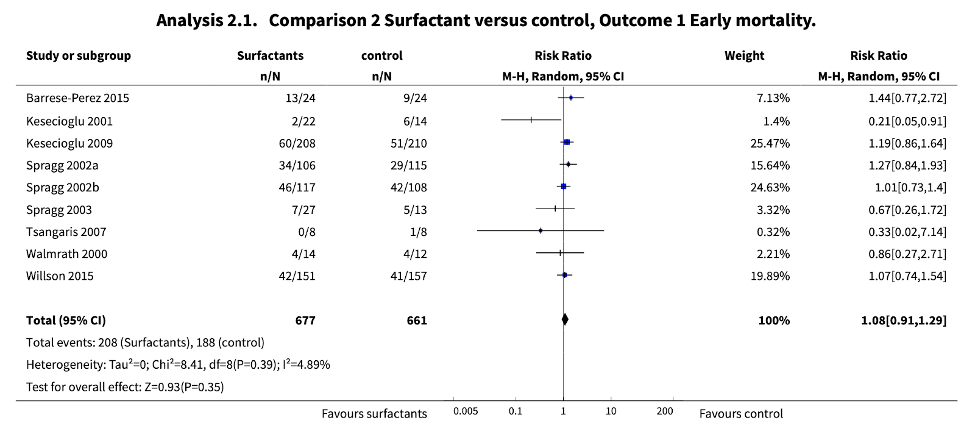
Figure 3
Meta-analysis of mortality data in ARDS after surfactant therapy (Lewis et al. 2019).
Another intriguing possibility is that the heterogeneity of ARDS as a clinical diagnosis has masked effects of surfactant therapy in subgroups who might specifically benefit. Notably, post hoc analyses of the Spragg 2004 NEJM cohort (a randomized, placebo-controlled trial of surfactant in ARDS) revealed a statistically significant interaction between mode of ARDS (direct versus indirect lung injury), indicating that surfactant-treated patients with primary pulmonary disease (aspiration or pneumonia) tended to have higher survival than those with ARDS arising as a consequence of other critical illness (Spragg et al. 2004). This observation is thought-provoking; if some forms of ARDS are driven primarily by surfactant dysfunction with pulmonary edema and hyaline membranes as secondary events, one might expect them to be particularly responsive to surfactant supplementation. On the other hand, if other forms of ARDS are driven primarily by systemic “capillary leak”, it is less clear that additional surfactant could address this defect. Some have also suggested directly measuring surfactant secretion rates and composition in patients to identify those who might benefit (Dushianthan et al. 2012). COVID-19, as a disease proposed (though not proven) to occur primarily through alveolar injury, might represent exactly the type of disease worth such study – an idea not lost on makers of synthetic surfactant (Reuters 2020). In fact, just two days ago, a clinical trial investigating surfactant in COVID-19 was posted on clinicaltrials.gov.
Concluding Thoughts
It is clear from decades of basic physiological studies, human genetics, and clinical neonatology literature that loss of surfactant activity in the human lung predisposes to disease states which share many features with what we now know as ARDS. Moreover, surfactant administration has proven safe and effective in neonatal RDS - thereby providing enticing proof-of-concept that at least some forms of ARDS may likewise be effectively treated. To date, trials of surfactant administration in adults have yet to bear fruit, but these negative results may well reflect technical or patient selection issues. COVID-19 represents an unexpected but potentially powerful opportunity to re-visit the therapeutic potential of administering exogenous surfactant and we look forward to clinical trial data as it becomes available.
References:
- Anzueto, A., R. P. Baughman, K. K. Guntupalli, J. G. Weg, H. P. Wiedemann, A. A. Raventós, F. Lemaire, W. Long, D. S. Zaccardelli, and E. N. Pattishall. 1996. “Aerosolized Surfactant in Adults with Sepsis-Induced Acute Respiratory Distress Syndrome. Exosurf Acute Respiratory Distress Syndrome Sepsis Study Group.” The New England Journal of Medicine 334 (22): 1417–21.
- Ashbaugh, D. G., D. B. Bigelow, T. L. Petty, and B. E. Levine. 1967. “Acute Respiratory Distress in Adults.” The Lancet 2 (7511): 319–23.
- Chen, C. T., T. J. Toung, and M. C. Rogers. 1985. “Effect of Intra-Alveolar Meconium on Pulmonary Surface Tension Properties.” Critical Care Medicine 13 (4): 233–36.
- Clark, D. A., G. F. Nieman, J. E. Thompson, A. M. Paskanik, J. E. Rokhar, and C. E. Bredenberg. 1987. “Surfactant Displacement by Meconium Free Fatty Acids: An Alternative Explanation for Atelectasis in Meconium Aspiration Syndrome.” The Journal of Pediatrics 110 (5): 765–70.
- Dushianthan, Ahilanandan, Rebecca Cusack, Victoria Goss, Anthony D. Postle, and Mike P. W. Grocott. 2012. “Clinical Review: Exogenous Surfactant Therapy for Acute Lung Injury/acute Respiratory Distress Syndrome--Where Do We Go from Here?” Critical Care / the Society of Critical Care Medicine 16 (6): 238.
- El Shahed, Amr I., Peter A. Dargaville, Arne Ohlsson, and Roger Soll. 2014. “Surfactant for Meconium Aspiration Syndrome in Term and Late Preterm Infants.” Cochrane Database of Systematic Reviews , no. 12 (December): CD002054.
- Filoche, Marcel, Cheng-Feng Tai, and James B. Grotberg. 2015. “Three-Dimensional Model of Surfactant Replacement Therapy.” Proceedings of the National Academy of Sciences of the United States of America 112 (30): 9287–92.
- Floros, Joanna, Neal J. Thomas, Wenlei Liu, Costas Papagaroufalis, Marietta Xanthou, Sunita Pereira, Ruzong Fan, Xiaoxuan Guo, Susan Diangelo, and Jelena Pavlovic. 2006. “Family-Based Association Tests Suggest Linkage between Surfactant Protein B (SP-B) (and Flanking Region) and Respiratory Distress Syndrome (RDS): SP-B Haplotypes and Alleles from SP-B-Linked Loci Are Risk Factors for RDS.” Pediatric Research 59 (4 Pt 1): 616–21.
- Granger, Robert A. 1995. Fluid Mechanics (Dover Books on Physics). 1st edition. Dover Publications.
- Lewis, Sharon R., Michael W. Pritchard, Carmel M. Thomas, and Andrew F. Smith. 2019. “Pharmacological Agents for Adults with Acute Respiratory Distress Syndrome.” Cochrane Database of Systematic Reviews.
- Lotze, A., G. R. Knight, G. R. Martin, D. I. Bulas, W. M. Hull, R. M. O’Donnell, J. A. Whitsett, and B. L. Short. 1993. “Improved Pulmonary Outcome after Exogenous Surfactant Therapy for Respiratory Failure in Term Infants Requiring Extracorporeal Membrane Oxygenation.” The Journal of Pediatrics 122 (2): 261–68.
- Lu, Qin, Mao Zhang, Cassio Girardi, Belaïd Bouhemad, Jozef Kesecioglu, and Jean-Jacques Rouby. 2010. “Computed Tomography Assessment of Exogenous Surfactant-Induced Lung Reaeration in Patients with Acute Lung Injury.” Critical Care / the Society of Critical Care Medicine 14 (4): R135.
- Marttila, Riitta, Ritva Haataja, Susan Guttentag, and Mikko Hallman. 2003. “Surfactant Protein A and B Genetic Variants in Respiratory Distress Syndrome in Singletons and Twins.” American Journal of Respiratory and Critical Care Medicine 168 (10): 1216–22.
- McCormack, Francis X., and Jeffrey A. Whitsett. 2002. “The Pulmonary Collectins, SP-A and SP-D, Orchestrate Innate Immunity in the Lung.” The Journal of Clinical Investigation 109 (6): 707–12.
- Meng, Haoyu, Ying Sun, Jun Lu, Shukun Fu, Zhaoyi Meng, Melanie Scott, and Quan Li. 2012. “Exogenous Surfactant May Improve Oxygenation but Not Mortality in Adult Patients with Acute Lung Injury/Acute Respiratory Distress Syndrome: A Meta-Analysis of 9 Clinical Trials.” Journal of Cardiothoracic and Vascular Anesthesia. https://doi.org/10.1053/j.jvca.2011.11.006.
- Meng, Shan-Shan, Wei Chang, Zhong-Hua Lu, Jian-Feng Xie, Hai-Bo Qiu, Yi Yang, and Feng-Mei Guo. 2019. “Effect of Surfactant Administration on Outcomes of Adult Patients in Acute Respiratory Distress Syndrome: A Meta-Analysis of Randomized Controlled Trials.” BMC Pulmonary Medicine 19 (1): 9.
- Neergaard, K. v. 1929. “Neue Auffassungen über Einen Grundbegriff Der Atemmechanik.” Zeitschrift Für Die Gesamte Experimentelle Medizin 66 (1): 373–94.
- Pérez-Gil, Jesús. 2008. “Structure of Pulmonary Surfactant Membranes and Films: The Role of Proteins and Lipid–protein Interactions.” Biochimica et Biophysica Acta (BBA) - Biomembranes 1778 (7): 1676–95.
- Polin, Richard A., Waldemar A. Carlo, Committee on Fetus and Newborn, and American Academy of Pediatrics. 2014. “Surfactant Replacement Therapy for Preterm and Term Neonates with Respiratory Distress.” Pediatrics 133 (1): 156–63.
- Reuters. 2020. “BRIEF-Windtree To Pursue Clinical Study Of Lung Injury Treatment In COVID-19 Patients With Its Kl4 Surfactant Therapy,” March 24, 2020. https://www.reuters.com/article/brief-windtree-to-pursue-clinical-study-idUSFWN2BH088.
- Rockx, Barry, Thijs Kuiken, Sander Herfst, Theo Bestebroer, Mart M. Lamers, Bas B. Oude Munnink, Dennis de Meulder, et al. 2020. “Comparative Pathogenesis of COVID-19, MERS, and SARS in a Nonhuman Primate Model.” Science, April. https://doi.org/10.1126/science.abb7314.
- Spragg, Roger G., James F. Lewis, Hans-Dieter Walmrath, Jay Johannigman, Geoff Bellingan, Pierre-Francois Laterre, Michael C. Witte, et al. 2004. “Effect of Recombinant Surfactant Protein C–Based Surfactant on the Acute Respiratory Distress Syndrome.” New England Journal of Medicine. https://doi.org/10.1056/nejmoa033181.
- Xu, Zhe, Lei Shi, Yijin Wang, Jiyuan Zhang, Lei Huang, Chao Zhang, Shuhong Liu, et al. 2020. “Pathological Findings of COVID-19 Associated with Acute Respiratory Distress Syndrome.” The Lancet. Respiratory Medicine 8 (4): 420–22.
- Zhang, Huilan, Peng Zhou, Yanqiu Wei, Huihui Yue, Yi Wang, Ming Hu, Shu Zhang, et al. 2020. “Histopathologic Changes and SARS-CoV-2 Immunostaining in the Lung of a Patient With COVID-19.” Annals of Internal Medicine, March. https://doi.org/10.7326/M20-0533.
Learn more about research in the Division of Pulmonary and Critical Care Medicine
View all FLARE content