Taper Corrosion in Total Hip Arthroplasty
In This Article
- Taper corrosion-related ALTR is an infrequent complication of THA
- A systematic approach in evaluating patients with ALTR is important to ensure a timely diagnosis
- Early detection can help improve revision-surgery outcomes for patients
Subscribe to the latest updates from Orthopaedics Advances in Motion
Hip and knee arthroplasties are among the most commonly performed surgeries in the United States. According to the CDC, over 300,000 total hip arthroplasties were performed on patients 45 and older in 2010. That number has more than doubled since 2000 and continues to rise, according to a 2012 study published in the Journal of the American Academy of Orthopaedic Surgeons. Modularity in total hip arthroplasty (THA) allows surgeons to optimize implant reconstruction to patient anatomy intraoperatively. The introduction of femoral stem head-neck modularity has been a mainstay design feature for over two decades. The so-called dual-taper THA implants possess interchangeable necks, providing additional modularity at the femoral neck-stem interface.
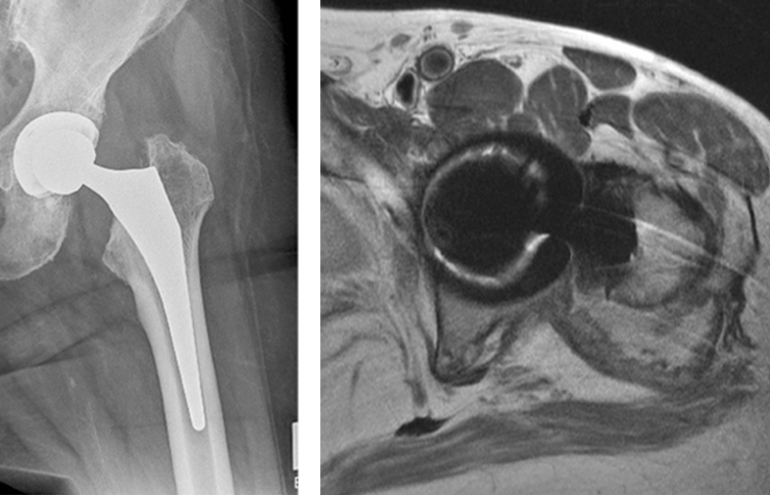
Fig. 1 (Left): A Radiograph of a 75-Year-Old Female Presenting with Increasing Hip Pain and Late Recurrent Dislocations at Four Years, with Metal-On-Highly Crosslinked Polyethylene THA
Fig. 2 (Right): A MARS MRI Demonstrating the Presence of Heterogeneous Complex Cystic Pseudotumor.
Recently, however, there is increasing concern regarding the occurrence of adverse tissue reactions in THA patients with metal-on-polyethylene bearings, due to corrosion at modular taper junctions (Figure 1). The reported prevalence of these adverse reactions ranges from 1-3% of modular THA patients, according to Young-Min Kwon, MBBS, PhD, FRACS, FRCS, an orthopedic surgeon at Massachusetts General Hospital.
Although adverse local tissue reactions (ALTR), or pseudotumors, were initially described as a complication of metal-on-metal bearings, the presence of ALTR in patients with taper corrosion is thought to result from corrosion at the modular taper junction, secondary to reciprocating movement at the modular junction. This leads to fretting corrosion in a process described as mechanically-assisted crevice corrosion (MACC).
Diagnosing ALTR
There should be a low threshold to conduct a systematic clinical evaluation of patients with painful modular THAs, as early recognition and diagnosis will ensure prompt and appropriate treatment.
“If you have a patient with unexplained pain or late recurrent dislocations without obvious cause after THA surgery, a differential diagnosis of taper corrosion–related ALTR should be considered,” says Dr. Kwon. “Based on the recent reports, taper corrosion–related ALTR is an infrequent complication. It is, however, important to have a systematic approach in evaluating these patients, to ensure they can be diagnosed in a timely manner.”
To address this problem, Dr. Kwon served on a task force of orthopedic surgeons from the American Association of Hip and Knee Surgeons, the American Academy of Orthopaedic Surgeons (AAOS) and the Hip Society. Published in the Journal of Arthroplasty in 2014, the task force discussed the issue and wrote consensus statements that included a systematic risk stratification algorithm that can assist in early recognition and diagnosis of ALTR.
Serum cobalt and chromium metal ion analysis with elevation beyond one parts per billion (ppb) and abnormalities in cross-sectional imaging modalities, such as metal artifact reduction sequence (MARS) MRI, are helpful in evaluating for taper corrosion–related ALTR (Figure 2). However, those making clinical decisions should avoid overreliance on any single investigative tool.
Revision Surgery Techniques and Outcomes
Revision surgery for taper corrosion necessitates a thoughtful systematic approach to reduce intra-operative complications. Meticulous and careful debridement must be performed to remove the pseudotumor while protecting neurovascular structures. The largest-diameter ceramic femoral head, which has a titanium sleeve compatible with the acetabular component, is used to maximize the head/neck ratio to optimize intra-operative stability. When indicated, removal of a well-fixed stem is technically challenging. Techniques such as trochanteric osteotomies, stack-pin techniques and top-out techniques have been described for stem removal, as documented in a 2016 study published in the Journal of Arthroplasty. The use of modular revision femoral implants, such as titanium modular tapered femoral stems, is frequently required to optimize intra-operative stability in the presence of extensive tissue necrosis.
Patients undergoing revision surgery are often concerned about the systemic elevation of metal ion levels and ask how long it will take to return to normal. A study by Dr. Kwon, presented at the AAOS meeting and published in 2016 in the Journal of Arthroplasty, showed that the metal ion levels in the vast majority of patients with elevated cobalt and chromium ion levels significantly decline following revision surgery. Serum cobalt and chromium levels decline, on average, by 32% and 21% at six weeks after revision surgery.
However, revision surgery may lead to increased complication rates and re-revision rates in the setting of significant adverse tissue reaction. Dr. Kwon's study found a high rate of early complications (20%) and re-revisions (8%) in 200 patients who underwent revision surgeries. The most common complication was dislocation, despite the use of large femoral head sizes, and the next most common was a recurrence of ALTR. Intra-operative tissue necrosis was correlated with the complication rate, suggesting the importance of early systematic evaluation of at-risk patients, including metal ion levels and MARS MRI, in optimizing revision-surgery outcome. Such diagnostic tools can assist in improving the detection and treatment of ALTR caused by taper corrosion.
Dr. Kwon concludes, "These complications can cause disabling pain, so surgeons need to evaluate patients with unexplained pain systematically. Early detection of taper corrosion ALTR can help to improve the revision-surgery outcomes for patients."
Learn about the Center for Hip and Knee Replacement
Refer a patient to the Center for Hip & Knee Replacement