Foot & Ankle Research and Innovation Laboratory Harnesses Weight-bearing CT Scans to Manage Instability
In This Article
- Assessment of foot and ankle instability using traditional imaging modalities can be impeded by imprecise measurements of bone morphology, alignment and joint spaces.
- The emerging technology of weight-bearing CT for foot and ankle imaging appears to overcome these limitations and is under evaluation at Massachusetts General Hospital
- Weight-bearing CT can also play a key role in the assessment of other, non- foot and ankle, orthopaedic lower extremity pathology
Subscribe to the latest updates from Orthopaedics Advances in Motion
Traditionally, orthopaedic subspecialties have used 2-dimensional imaging measurements for diagnosing and managing musculoskeletal pathology.
Now, this is changing at Massachusetts General Hospital thanks to innovative research and clinical applications refining and harnessing the technology of the cone-beam, weight-bearing computed tomography (WBCT) imaging at the Foot & Ankle Research and Innovation Laboratory (FARIL), led by Christopher W. DiGiovanni, MD, chief of the Foot and Ankle Center at Mass General, and Bart Lubberts, MD, PhD, director of research and development in FARIL.
"Our combined focus is on integrating education, technology and innovation to make FARIL a platform for truly innovative, patient-focused solutions," says Dr. Lubberts. "Much of the clinical decision-making in musculoskeletal disease relies not on the static views taken by radiographs, MRI or conventional CT scans, but in the ability to apply stress and manipulate bones, joints and ligaments while under direct visualization by imaging."
About Weight-bearing CT
During an orthopedic foot and ankle WBCT scan, a patient stands on a platform with both feet side by side. The WBCT scanner makes a single circumferential pass halfway up the tibia and exposes the patient to substantially lower doses of radiation than earlier CTs because the design shields against radiographic scatter.
Because the patient is standing and bears weight, the scan can capture malalignment of anatomic structures or skeletal movement related to musculoskeletal injury. For example, in patients suffering a high ankle sprain, it may reveal separations of the distal fibula and tibia and increased joint volume relative to the contralateral healthy side. Such findings suggest ankle syndesmosis instability related to ligamentous injury.
As diagnostic instability measures play an important role in the treatment decision process, FARIL prioritizes imaging modalities that can assess and evaluate the instability of the foot and ankle. These include WBCT, dynamic portable ultrasound and diagnostic arthroscopy to which load or manual stress can be added. WBCT has the advantage of providing a three-dimensional image of bones in their functional position and allow a view of the contralateral ankle as an internal control.
"Adding weight to the analysis is key to getting a full understanding of instability and musculoskeletal function so surgeons can optimize treatment based on that understanding," Dr. Lubberts says.
Mass General is one of the few U.S. medical and research facilities to offer this newest generation of orthopedic imaging. Dr. Lubberts is encouraged by preliminary results and hopes the model can extend to other orthopaedic subspecialties within the hospital.
"Weight-bearing CT can play a key role in the assessment of other orthopedic lower extremity pathology as well," he says.
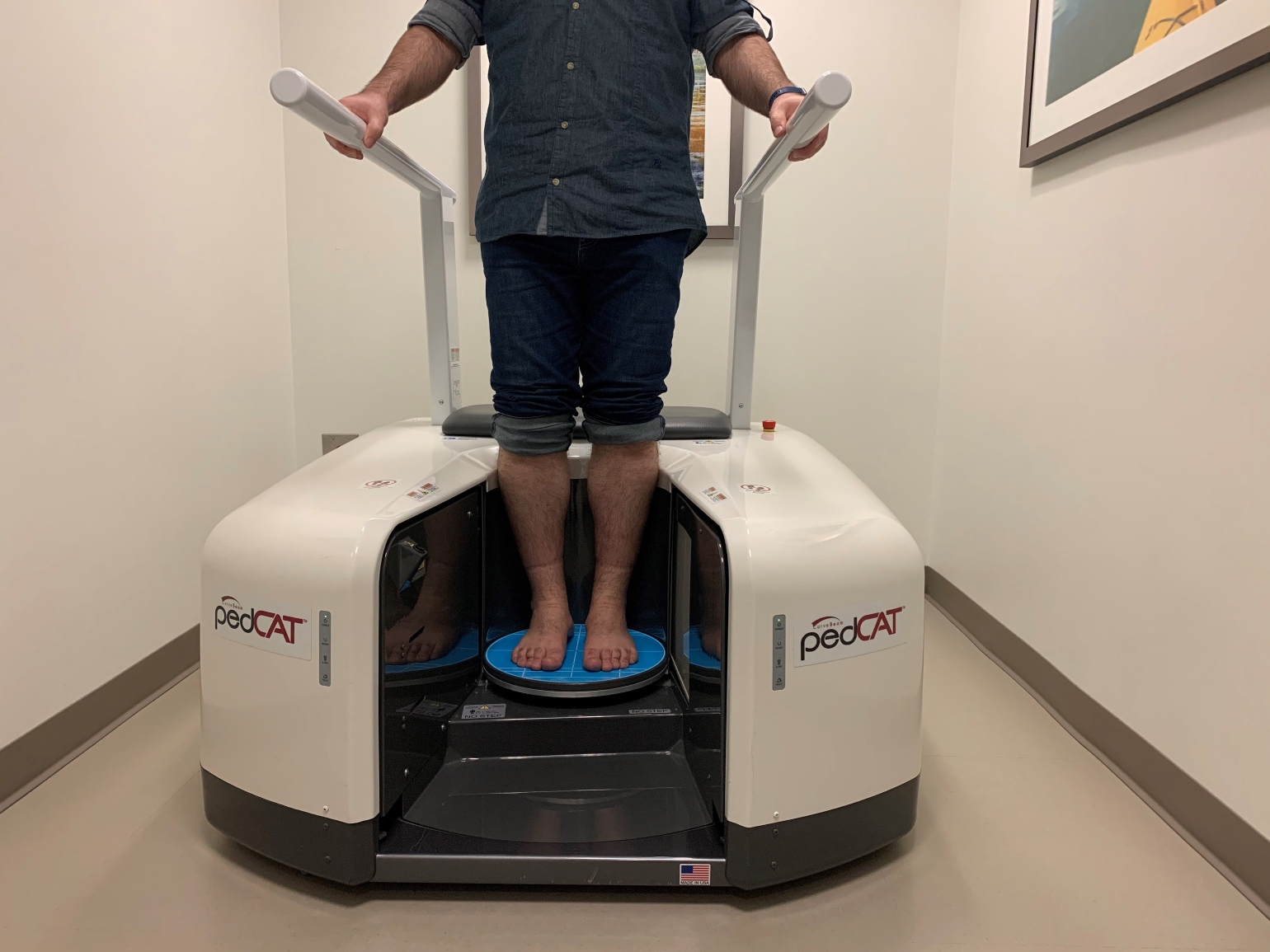
Figure 1
A FARIL research fellow demonstrates the use of WBCT in the clinic.
FARIL Research Highlights
The conditions FARIL is investigating with WBCT and other technologies are comparative instability and injury imaging on cadavers and arthroscopic instability assessment.
The team is comparing dynamic portable ultrasound exam data on cadaveric specimen with injuries previously assessed with conventional CT, MRI or fluoroscopy to make new instability measurements. For example, in the case of high ankle strains, MRI may reveal a torn or strained ligament. To replicate it, the dynamic portable ultrasound exam may require multiple anatomic position adjustments.
"We have to determine the best anatomical location, put manual stress on the ligament and see movement in the joint and then measure the distance and direction of the movement," says Dr. Lubberts.
Integrated, Multidisciplinary Team
The tightly integrated multidisciplinary FARIL team meets weekly to share reports from both the research lab and the patient clinic, and in that way, improve both enterprises.
"These care-provider and researcher meetings are really important. Not only do you have original research with input from what physicians are seeing in patients, but you have it directly implemented into patient care. It's the best of both medical worlds," says Dr. Lubberts.
Through its creative interdisciplinary relationships, the team considers problems ranging from devising an improved shoe insole for first metatarsophalangeal arthritis patients, to preventing post-surgical pulmonary embolisms and deep vein thrombosis in foot and ankle patients.
Dr. Lubberts is encouraged by FARIL's interdisciplinary biomechanical and clinical research model and its emphasis on education, innovation and technology. He hopes to encourage his Mass General orthopedic colleagues to consider it.
"One of the things I've learned," he says, "is that you have to start small with the things you have, and show success. I think we've shown it's a successful platform, and it's time to expand."
Learn more about the Foot and Ankle Research and Innovation Lab
Refer a patient to the Department of Orthopaedics at Mass General