Incidence of Ocular Burns Increasing in U.S.
Key findings
- This retrospective registry-based study investigated the incidence and outcomes of chemical and thermal ocular burns in the U.S. along with demographic risk factors
- Between 2013 and 2017, 65,906 cases of ocular burns were reported in 64,760 patients and the incidence significantly increased by 20% during that period
- Ocular burns afflicted men and women at similar rates and the average patient age was older than previously reported: 45 and 52 for men and women, respectively
- Despite a decrease in vision in the short term after the burn, on average there was no significant long-term loss of visual acuity or increase in intraocular pressure
- For care related to the burn, the average number of office visits per patient was 1.5 (range, 1–22)
Because ocular burns are relatively infrequent, little epidemiologic information has been available. Jia Yin, MD, PhD, MPH, Joan W. Miller, MD, and Alice Lorch, MD, MPH, of the Department of Ophthalmology at Mass Eye and Ear/Mass General Hospital, and colleagues recently conducted a registry-based U.S. study that upends the concept of who is at risk for ocular burns—and shows an increase in incidence over recent years. Their report appears in The Ocular Surface.
Subscribe to the latest updates from Ophthalmology Advances in Motion
Study Methods
Mass Eye and Ear was one of four academic groups selected nationwide and awarded unique access to the American Academy of Ophthalmology's Intelligent Research in Sight (IRIS®) Registry—the nation's first electronic health record-based comprehensive eye disease and condition registry. Using this registry, which now contains data on more than 71 million patients, the researchers identified new chemical or thermal ocular burn diagnoses between January 2013 and December 2017.
Incidence
- During the study period 65,906 cases of ocular burns were reported in 64,760 patients (average 13,181 cases/year)
- The incidence increased 20% from 2013 to 2017 (from 65 to 78 new cases per 100,000 new diagnoses; P=0.03)
Demographics
- The cohort included 32,337 men (50%) and 32,226 women (50%)
- The average age at diagnosis was 45 in men and 52 in women (P<0.001); for both sexes that is older than has been reported previously
Laterality
Laterality was unspecified for 52% of cases. Of the 31,534 cases with specified laterality, 72% were unilateral.
Outcomes
As expected, acute ocular burns resulted in substantial short-term loss of visual acuity. However, most of the loss was recovered—there was no significant change in visual acuity when measurements were compared for the year prior to the burn and the year of the last visit. There were no significant long-term changes in average intraocular pressure.
For care related to the burn, the average number of office visits per patient was 1.5 (range, 1–22).
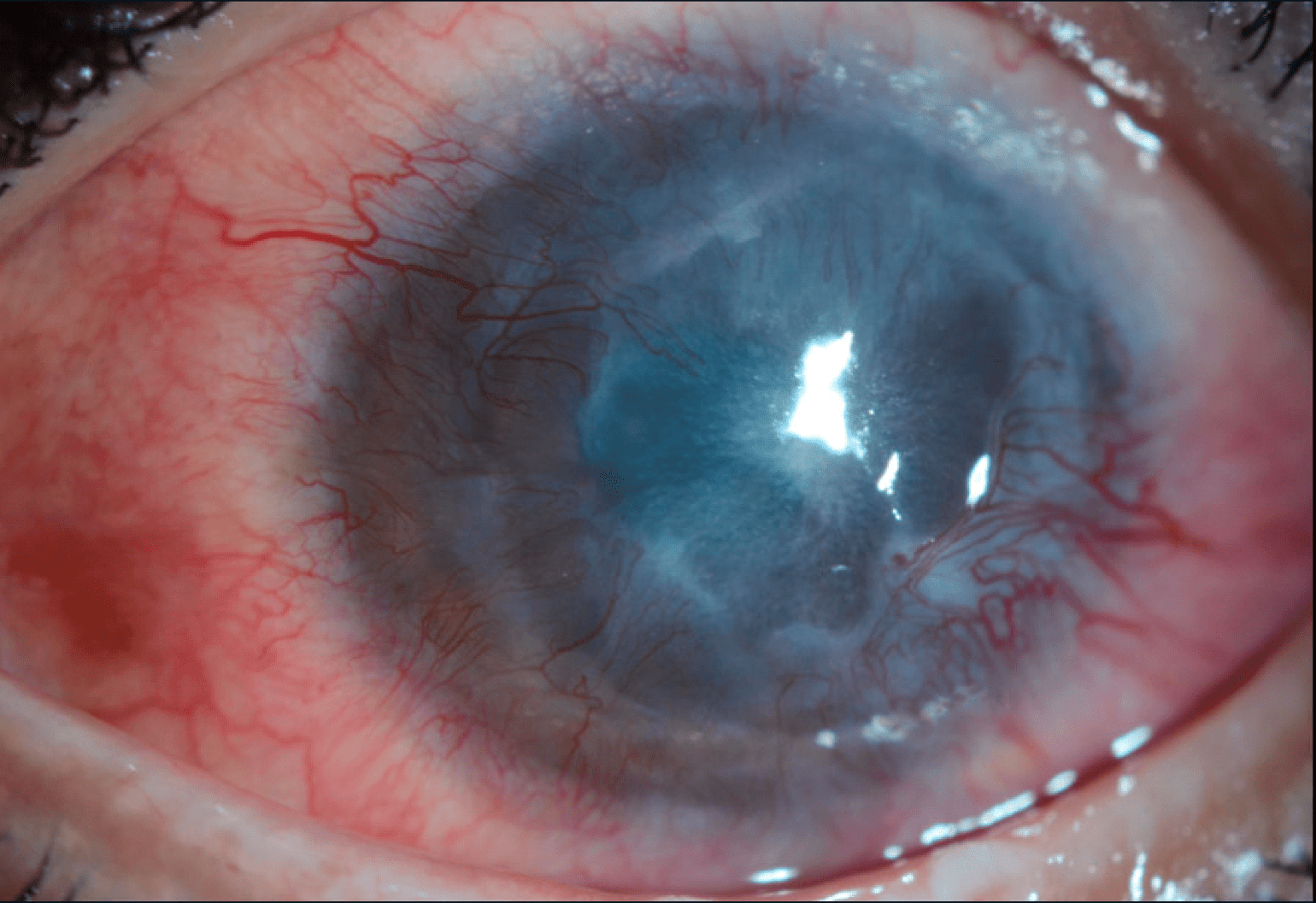
Figure 1
An example of an ocular burn due to a chemical injury. The patient was treated at Mass Eye and Ear by Jia Yin, MD, PhD, MPH. Image courtesy of Dr. Yin.
Commentary
Young men are traditionally considered the population at greatest risk of ocular burns, but this study suggests the reality is different, at least in the U.S. It's reassuring that the great majority of chemical and thermal ocular burns are unilateral, require only modest follow-up and result in no significant long-term loss of visual acuity or increase in intraocular pressure.
view original journal article Subscription may be required
Learn more about the Department of Ophthalmology at Mass Eye and Ear/Mass General
Refer a patient to Mass Eye and Ear/Mass General