Tracking Outcomes in Proton Therapy for Cancer
In This Article
- Massachusetts General Hospital was one of the first institutions to use proton beam therapy to treat cancer
- Two centers at the main hospital campus are among few in the nation to offer this advanced, targeted radiation treatment
- Mass General clinician-researchers are leading efforts to understand which patients can benefit most from proton beam therapy
- Studies are also tracking long-term outcomes and quality of life
Massachusetts General Hospital was one of the first institutions in the world to use proton therapy, which can deliver radiation therapy with fewer side effects and with a higher radiation dose if needed to treat cancer. It remains one of the few institutions to offer this targeted therapy. Now, Mass General researchers are furthering the field by examining long-term outcomes and elucidating which patients can benefit most from proton beam therapy.
Subscribe to the latest updates from Cancer Center Advances in Motion
"With any new technology or treatment, we have a social responsibility to participate in and lead studies to guide best practices," says Helen Shih, MD, medical director of the Proton Therapy Centers at the Mass General Cancer Center. "How else will the rest of the world understand what this opportunity is? Whether you're a patient who's trying to read about it, a provider who's trying to figure out whether they should refer a patient, an insurance carrier who's wondering whether you should pay for this different technology that is more expensive—those data are fair to request."
With the resources of two proton therapy centers, Dr. Shih and colleagues use the advanced technology to treat patients with certain cancers. They also design and conduct studies to improve proton therapy.
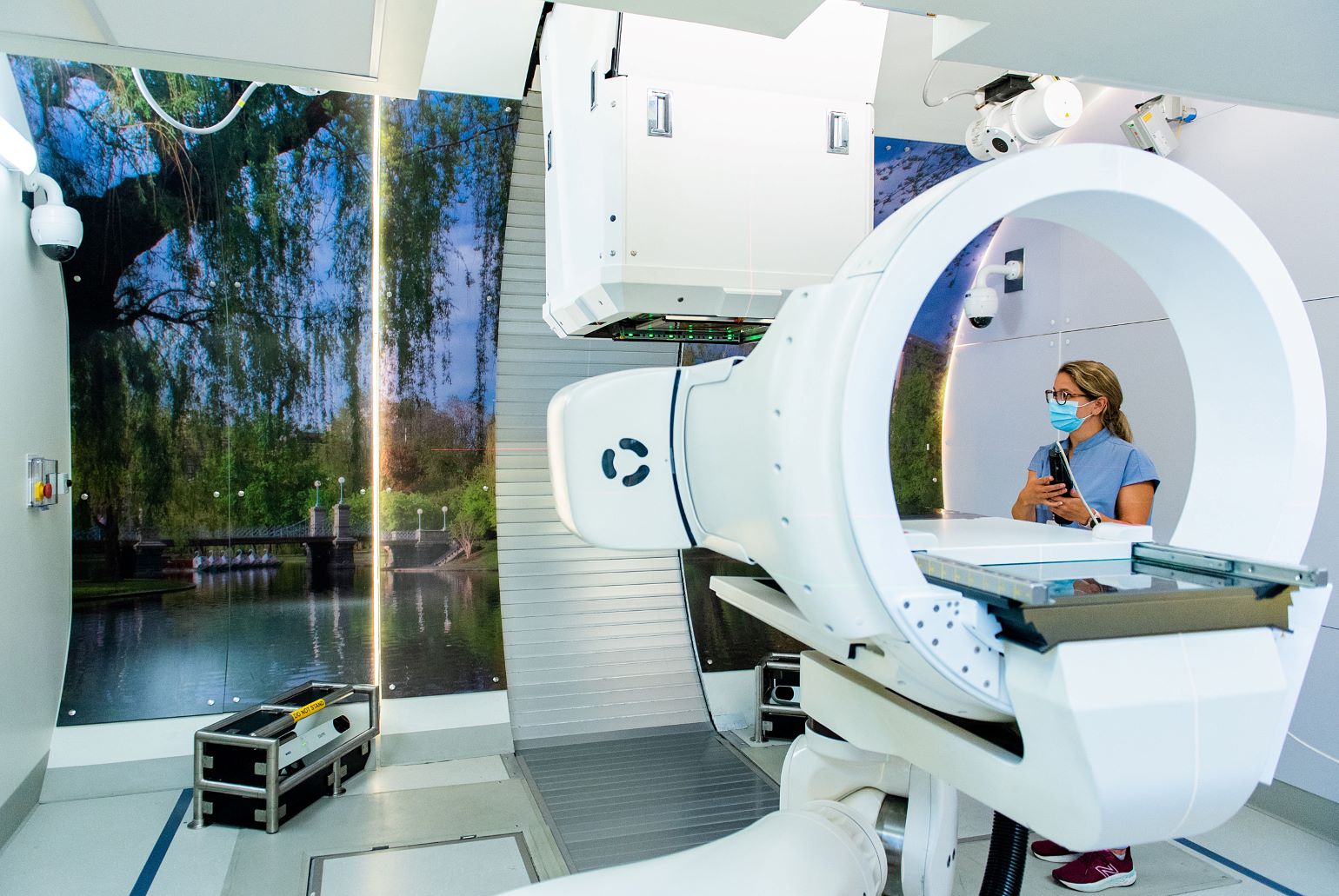
Figure 1
The proton therapy machine located in the Gordon-Browne Proton Therapy Center.
Proton Beam Therapy Versus Photon Therapy
Proton therapy uses protons, which are positively charged particles, to treat various cancers. It's delivered daily (Monday through Friday) most commonly for between three to eight weeks, sometimes concurrently with chemotherapy or other types of treatments.
The technology may confer some benefits over traditional photon radiation. "Photons, what 99% of the world uses, are high-energy X-rays. There's no mass. There's no charge. It's just a bundle of energy that travels through air into a patient, and through their body. We can direct a photon beam, but once we let it go, we can't steer it anymore," Dr. Shih explains.
Photon beams can damage nearby tissues, and they continue to deliver radiation as they leave the body. That can cause adverse side effects, even many years later.
Protons offer an innovation in cancer therapy by focusing radiation to travel to a specific depth into the body, where it then stops. A proton beam delivers a targeted dose of radiation directly to the tumor or desired target—but very little radiation to surrounding tissues. This precision can minimize early and late side effects and permit higher doses to be delivered safely.
"Because a proton beam has a charge, we can steer it with magnets and direct it to where we want to deliver radiation," Dr. Shih says. "It's like a lollipop. The little stick is a beam containing a bundle of protons, which travels a finite distance into tissues, and then the beam stops. A little bit of radiation hits your skin, and the beam does give some radiation to the tissues it travels through as it penetrates to the target area. It then delivers this wallop of radiation at the target—that's the candy of the lollipop. And then the beam stops."
Understanding When to Use Proton Therapy for Cancer
In many cases, proton and photon therapy may be relatively equal, Dr. Shih says. But proton technology involves greater technical hardware and software to achieve precision. The therapy is costly, requires expertise and is available only at select institutions. So it's important to understand which patients can benefit most before recommending it.
"We have to be thoughtful about where the margin of benefit is. We often heavily rely on our medical physicists and medical dosimetrists to better understand the technologies and feasibility of treatment plans to better assess which system makes more sense for each patient," Dr. Shih explains. "And if there are certain circumstances where we believe there would be a big difference, then we'll push for protons."
Proton Therapy for Pediatric Cancer
In addition to treating patients, Dr. Shih and colleagues are conducting research to define when proton therapy is most beneficial. Among the populations who can benefit most are children with cancer. Radiation can affect growth, development, cognitive function, and risk of future cancer. But if you minimize radiation exposure with proton therapy, you can minimize those risks, Dr. Shih says.
Mass General leads the Pediatric Proton Consortium Registry (PPCR), a multi-institution database that tracks outcomes in pediatric patients receiving this type of therapy. The PPCR facilitates access to proton therapy and provides important data for outcomes research.
Proton Therapy for Brain Tumors
Proton therapy is also particularly useful for brain tumors in patients of all ages. "The brain is what makes us human—our ability to think, feel, laugh, love and appreciate family and friends. If you lose those abilities, that's such a significant impact," Dr. Shih says. "And we know when we treat the whole brain, we can see accelerated aging, effects on cognitive processing, some features like dementia, even personality changes. We can reduce that by reducing the amount of radiation to the brain."
Current brain tumor patients receiving proton therapy are offered the opportunity to participate in studies either specific to their tumor type or simply for receiving proton therapy to the brain to assess our ability to preserve cognitive function and other functions such as hearing and vision in addition to surveying patient views on their quality of life.
Proton Therapy Research in Other Cancer Types
The Mass General Cancer Center examines the role of proton therapy in several disease sites. For example, trials are exploring:
- Brain tumors, aimed to show the preservation of cognition, vision, and other functions. NCT03286335
- High grade meningiomas, treated at higher dose for better tumor control—in collaboration with MD Anderson Cancer Center. NCT02693990
- IDH-mutant lower grade gliomas, randomized between photons and protons to assess better cognitive preservation. Sponsored by NRG Oncology. NCT03180502
- Breast cancer, randomized between photons and protons to assess radiation damage to the heart and other tissues. NCT02603341
- Esophageal cancer, randomized between photons and protons. Sponsored by NRG Oncology. NCT03801876
- Liver cancer, randomized between photons and protons. Sponsored by NRG Oncology. NCT03186898
- Lung cancer, randomized between photons and protons. Sponsored by NRG Oncology. NCT01993810
- Sarcomas of the retroperitoneum, to assess safety and effectiveness. NCT01659203
- Pediatrics, multiple studies across different tumor types such as neuroblastoma, NCT02112617, and rhabdomyosarcoma, NCT00592592
- Prostate cancer, randomized between photons and protons to assess preservation of quality of life and function (for example, urinary, rectal, and erectile). This study has now completed accrual, with results maturing.
Referring a Patient for Proton Therapy
Mass General has two proton centers on the main campus in Boston: the Francis H. Burr Proton Therapy Center and the Gordon-Browne Proton Therapy Center. Dr. Shih encourages medical colleagues to reach out to learn more about proton therapy for cancer treatment. She and her team can help determine whether it may benefit certain patients with cancer or other indications for radiation treatment.
"We're lucky at Mass General to have such a large volume of patients and all the different permutations of specializations. Proton radiation is a different technology that may afford benefits in terms of reducing side effects for some patients," she says. "It's worth a thoughtful discussion between the referring physician and a radiation oncologist who is an expert with protons to figure out whether or not there is an added value to the technology for that specific patient."
Learn more about proton therapy at the Mass General Cancer Center
Refer a patient to the Mass General Cancer Center